The Role of Hard and Soft Tissue Grafting in Successful Implant Outcomes
Key Takeaways:
- Grafting Boosts Implant Success: Hard- and soft-tissue grafts improve stability, function, and aesthetics.
- Hard Tissue: Restores bone for secure implant placement using various graft types.
- Soft Tissue: Enhances gum health, prevents recession, and supports natural appearance.
- Combined Approach: Often needed in complex cases for predictable outcomes.
- Innovation & Planning: New materials and personalized treatment optimize healing and long-term results.
Introduction
Advancements in dental implantology have transformed restorative dentistry, enabling practitioners to deliver highly functional, natural-looking solutions to patients with missing teeth. Despite these advancements, the predictability and stability of dental implants remain closely linked to the health and availability of the surrounding hard and soft tissues at the implant site. Contemporary grafting techniques are vital for optimizing the biological environment and supporting the longevity and appearance of implants. For dental teams seeking further expertise in comprehensive implant procedures, organizations such as the Pikos Institute offer training and resources to enhance practitioner skill sets.
Understanding why grafting is essential requires recognizing its effect on clinical outcomes. Dental professionals employ grafting procedures to facilitate the best possible environment for osseointegration (the direct structural connection between bone and implant). This foundation is often compromised in cases of periodontal disease, trauma, or long-standing tooth loss, where bone or soft tissue volume is reduced. Through targeted hard- and soft-tissue augmentation, clinicians can rehabilitate the implant site, establishing optimal function and esthetics for the patient.
Understanding Hard Tissue Grafting
Hard tissue grafting refers to the restoration or augmentation of bone in the jaw, creating a robust foundation for implant placement. It is most commonly indicated in cases where natural bone has been lost to infection, trauma, or atrophy following tooth extraction. The main goal is to enable secure anchorage for dental implants and to recreate the ideal anatomic configuration required for function and esthetics.
Guided bone regeneration (GBR) is a leading technique in hard tissue grafting. By using biocompatible membranes to contain bone graft material at defect sites, clinicians promote new bone formation while preventing soft-tissue interference. The process enables bone volume regeneration, which is essential to support the planned implant. Autogenous bone (harvested from the patient), allografts, xenografts, and synthetic substitutes are all viable graft sources, each selected according to the clinical scenario and patient preference.
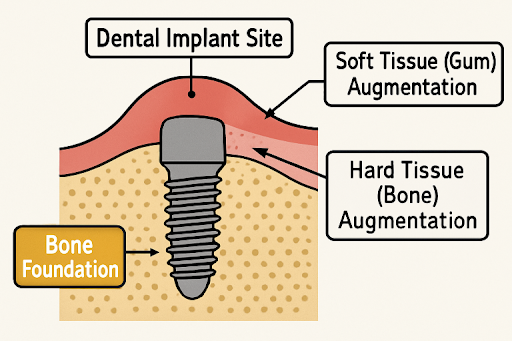
Soft Tissue Grafting: Enhancing Aesthetics and Function
While bone provides the foundation for dental implants, soft tissue health is just as critical for successful clinical and aesthetic outcomes. Soft tissue grafting aims to augment or reconstruct the gum tissue around implants. Thin or inadequate soft tissue can lead to unsightly recession, increased risk of infection, and compromised long-term outcomes. Connective tissue grafts and free gingival grafts are commonly used procedures to increase the width of keratinized tissue and reinforce the mucosal seal around the implant.
Strong peri-implant soft tissue not only protects the underlying bone from pathogenic bacteria but also contributes to the natural appearance of the implant site by mimicking the gum contour around natural teeth. This is particularly important in the aesthetic zone, where even subtle discrepancies can be noticeable. Results from clinical case series underscore that well-executed soft-tissue grafting reduces the incidence of peri-implant complications and helps ensure the success of the restorative and prosthetic phases of treatment.
Combining Hard and Soft Tissue Grafting
Many complex cases require a combination of hard and soft tissue grafting to address multifactorial tissue deficiencies. An integrated strategy enables simultaneous augmentation of bone and soft tissues, thereby maximizing the likelihood of a stable, esthetic implant outcome. This multidisciplinary approach is often necessary in cases of congenital defects, advanced periodontal disease, or major trauma. Coordinating procedures may also reduce overall treatment timelines and patient morbidity while producing a harmonious and functional result.
Clinical Evidence Supporting Grafting Procedures
Extensive clinical research supports the integration of bone and soft tissue grafting in implantology. For example, a randomized clinical trial found that bone grafting improved both hard and soft tissue parameters, especially in scenarios involving immediate implant placement. The findings suggest that while some clinical scenarios may demonstrate similar outcomes with or without grafting, the consistency and predictability of grafted sites are often superior in challenging cases.
Advancements in Grafting Materials and Techniques
The landscape of dental grafting materials and methods continues to evolve rapidly. Innovations such as bioactive glass composites have demonstrated accelerated bone ingrowth during the healing phase. Additive manufacturing and the combination of titanium alloys with bioactive agents are producing superior integration results and reducing healing times for patients. Clinicians are encouraged to keep abreast of such developments to provide the highest standard of care.
Patient Considerations and Treatment Planning
Every grafting procedure must be tailored to the individual patient. A comprehensive assessment should consider systemic health status, habits like smoking, oral hygiene, and aesthetic expectations. Digital imaging and diagnostic techniques are integral to modern planning processes, allowing for precise measurement of tissue deficits and risk assessment. Interdisciplinary collaboration and transparent patient communication are imperative to ensure optimal case selection, informed consent, and satisfaction with the final result.
Final Thoughts
Successful dental implant therapy increasingly relies on the proactive management of both hard and soft tissues through grafting procedures. By optimizing both function and esthetics at the implant site, these interventions improve clinical outcomes and elevate patient satisfaction. As evidence and technology continue to advance, the integration of strategic tissue grafting remains a cornerstone of contemporary implant dentistry, supporting the best possible outcomes for all patients.
